نبذة عن مركز عبدالكريم بكر الطبي
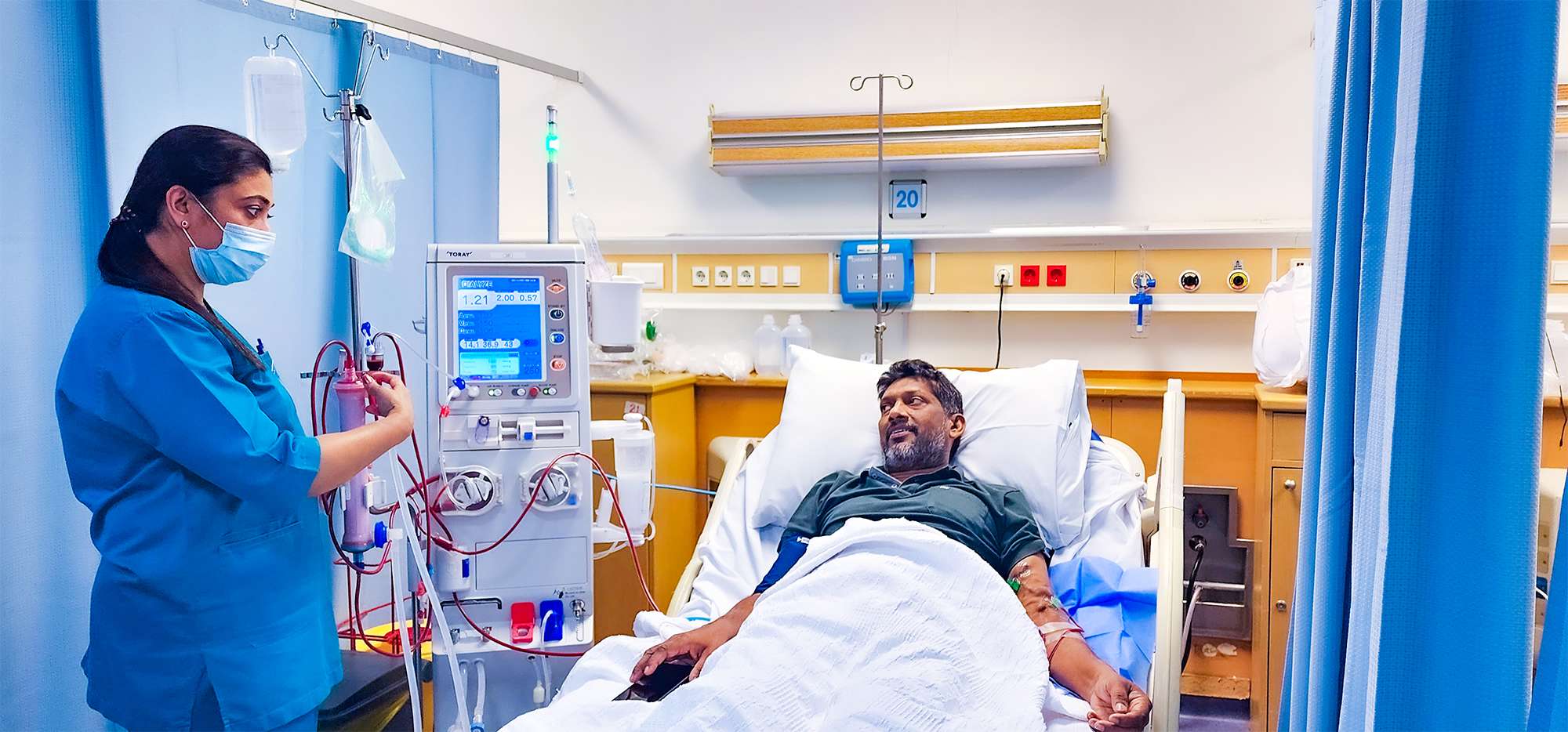
يقع مركز عبد الكريم بكر الطبي لغسيل الكلى غرب جمعية البر الخيرية بحي الزهراء بمدينة جدة. وقد أنشأه الشيخ عبدالكريم بكر – يرحمه الله – باعتباره مركزاً غير ربحي لعلاج مرضى الفشل الكلوي، وتكفّل بكامل تجهيزاته الطبية وغير الطبية، رغبة منه في خدمة المجتمع بأسس حديثة، والمساهمة في تخفيف معاناة مرضى الفشل الكلوي. وقد تم افتتاح هذا المركز المميز في الرابع من شهر رمضان المبارك ١٤٢٨هـ الموافق السادس عشر من شهر سبتمبر ٢٠٠٧م.
جوهرة جسمك هي كليتك
أحدث الأخبار
دكتور/ محمد غلاييني
الحمد لله رب العالمين الذي يسر لنا هذه الطريقة في العلاج و هو الغسيل الدموي الحمد لله الإنسان يستطيع بعد المعاناة قبل الغسيل و بواسطة هذا الغسيل أن يمارس حياته الطبيعية و الحمد لله.
دكتورة/ زكية فلمبان
الناحية الصحية لدرجة انه الإنسان لمن يداوم على الغسيل إللي هو الغسيل الدموي بيحس انه إيش أكتر بعد الغسيل براحة كبيرة و إزالة السموم من الجسم فالإنسان لا يعني يقول بأغسل أو ما بغسل لا ,يداوم عليه حتى يرتاح.